Mrs Scott had an endoscopy performed for iron deficiency anaemia. The endoscopy showed:
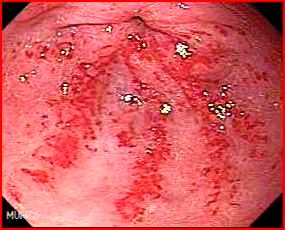
What is the diagnosis?
Watermelon stomach or GAVE (Gastric antral vascular ectasia).
GAVE is characterised by red patches or spots in either a diffuse or linear array in the antrum of the stomach. The red stripes represent ectatic and sacculated mucosal vessels.
It is called watermelon stomach because the streaky long red areas radiating out from the pylorus resemble the markings on watermelon.
Discuss the clinical manifestations of GAVE?
- It affects mostly women in their middle ages (usually with autoimmune disease like scleroderma etc)
- The most common clinical presentation is iron deficiency anaemia which may need blood transfusions.
- GAVE can also present with haematemesis or melaena.
Discuss the need for biopsy?
Watermelon stomach may be confused with severe antral gastritis and portal hypertensive gastropathy. Histology is not necessary to diagnose GAVE, which is made endoscopically, but their presence helps differentiate GAVE from other two conditions. GAVE histologically shows:
- Ectasia of mucosal capillaries
- Intravascular fibrin thrombi
- Fibrohyaline deposition around the ecstatic capillaries
- Spindle cell proliferation in the lamina propria
Discuss the aetiology of GAVE?
The aetiology of GAVE is unknown. Some authors suggest that intermittent obstruction of submucosal blood vessels caused by the prolapse of antral mucosa through the pylorus (caused by gastric contractions) lead to acquired vascular ectasia.
What are the causes of GAVE?
- Most cases of watermelon stomach are idiopathic. However, it has been associated with cirrhosis in 30% of cases. (It is present in 3% of cirrhotics, whereas 30% of GAVE patients have portal hypertension).
- In the setting of cirrhosis, GAVE syndrome can be difficult to differentiate from portal hypertensive gastropathy (PHG). This distinction is paramount in that PHG generally responds to a reduction in portal pressures whereas those with GAVE syndrome and coexisting portal hypertension generally do not respond to such therapy.
- GAVE syndrome can be distinguished from PHG in that GAVE generally has more antral involvement and the classic features of GAVE syndrome including gastric ectasia, gastric dilation, thrombi, increased spindle cell proliferation, and fibrohyalinosis may be seen on biopsy.
Discuss the management of GAVE?
In many cases iron replacement may be sufficient.
The treatment options in transfusions dependent GAVE are:
- Endoscopic treatment: APC has been found to improve lesions and decrease transfusion requirement. It has become the treatment of choice. It needs a median of 4 APC sessions to reduce transfusion requirements. Asymptomatic ulcers commonly occur following therapy, hence 2 weeks are allowed between sessions to allow the ulcers to heal.
- Surgical- Surgical antrectomy can cure the disease permanently. APC may not suffice in diffuse GAVE and surgery may be needed
- Medical: Oestrogen-progesterone combination treatment and tranexamic acid have been shown to be effective in case reports. However, the use of tranexamic acid is not without risk as there have been reports of ischaemic episodes and pulmonary embolus with the use of this agent.
Image coutesy of www.gastrointestinalatlas.com






