PEG insertion
Discuss the contraindications for PEG insertion?
Contraindications
INR>1.5, Platelets <50,000
Severe erosive gastritis or ulcer should be healed before PEG insertion
No longer considered as contraindications
- Lack of diaphanoscopy (transillumination of the endoscopic light through the abdominal wall) at the puncture area is no longer a contraindication;
- a negative needle aspiration test (using a syringe containing 5ml saline solution, puncture under continuous aspiration towards the air-filled stomach without prior air aspiration) is safer than an adequate diaphanoscopy
- Mild- Moderate ascites- Moderate ascites should be drained dry prior to PEG placement. Repeated paracentesis should be performed to keep the peritoneal cavity dry until the PEG tract has healed (usually in 2 weeks). Consider using antibiotics during this period to prevent seeding of the ascitic fluid
- Ventriculoperitoneal shunt
- Peritoneal dialysis
- Crohn’s disease
- Previous GI surgery (Billroth I or II resection or total gastrectomy)
- Concomitant administration of immunosuppressant’s.
Discuss PEG insertion?
- Radiological evidence of pneumoperitoneum may occur in more than 50% of cases; nevertheless, a pneumoperitoneum is not regarded as a complication. Even in cases of pneumoperitoneum and abdominal pain the patients first should be treated conservatively since severe cases are definitely rare and many unnecessary exploratory investigations have been described.
- It is not necessary to give a single, prophylactic dose of an antibiotic if the patient is already receiving antibiotic therapy.
- As a general rule it is advisable to use PEG tubes with a large lumen (at least 15 Charrie`re)—even in children—as smaller diameter tubes are associated with higher rates of clogging.
- Delivery of nutrients via the tube can commence within 1-2h after PEG placement.
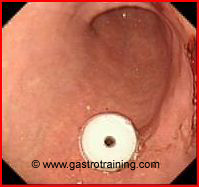
Discuss PEG buttons?
- Indications for PEG buttons:
- Cosmetic- aesthetically pleasing especially for the ambulatory patient. It lies flat against the stomach, and an external extension set is attached to the tube when administering formula or fluids.
- Mentally challenged or neurologically impaired patients- button design makes it intrinsically difficult for them to remove it inadvertently
- The switch from a PEG tube to a button can be made once the original PEG tube has been in place for a minimum of four weeks. Gastrostomy buttons are generally are made of polyurethane or silicone, and have a balloon, mushroom tip or disk to secure them internally.
- The one-step button (OSB) gastrostomy has been a useful modification of the PEG technique that allows for the initial placement of the button. Use of OSB has not been widespread possibly due to a lack of familiarity with the device and/or a high rate of previously reported complications (especially button migration, leakage and peritonitis). However, since button systems are much more expensive and have to be routinely exchanged approximately every 6 months because of material fatigue, these systems are usually only indicated for cosmetic reasons in socially fully integrated younger patients
- Currently available OSB
- Freka Pexact
http://www.fresenius-kabi.co.uk/internet/kabi/gb/fkintpub.nsf/Content/Product+Features+Freka+Pexact
- AMT PEG Assist™ Initial Placement Gastrostomy Kit
Discuss PEG tube removal?
- The standard method of removing percutaneous endoscopic gastrostomy (PEG) tubes is by repeat gastroscopy and retrieval of the internal PEG bumper by the oral route.
- PEG Tubes can be removed by external traction, if so designed.
- In adult patients with no risk of distal adhesions or strictures, gastrostomy tubes with rigid internal fixation devices can be removed by cutting them off close to the skin, pushing them into the stomach, and allowing them to pass spontaneously (http://www.bsg.org.uk/pdf_word_docs/enteral.pdf)
Patient can eat immediately after removal of a PEG tube
Pic 1 Corflo bumper
Ref






